Beautiful fall days call for beautiful fall activities. This weekend, SWIMBO and I headed to Williams Canyon outside of Manitou Springs. Day one --- HIKE IT!
Thursday, September 29, 2011
Monday, April 25, 2011
Gambling with Matches
 "Match Day" came and went this year on March 17th; I find it interesting to look at the raw data from the residency match, as it gives one an idea of what the next generation of physicians are thinking about the future, and my chosen specialty in particular. It is also instructive to see what is put out as PR for the match and compare it to the match results themselves:
"Match Day" came and went this year on March 17th; I find it interesting to look at the raw data from the residency match, as it gives one an idea of what the next generation of physicians are thinking about the future, and my chosen specialty in particular. It is also instructive to see what is put out as PR for the match and compare it to the match results themselves:
For Second Year, More U.S. Medical School Seniors Match to Primary Care Residencies
For the second year in a row, more U.S. medical school seniors will train as family medicine residents, according to new data released today by the National Resident Matching Program (NRMP). The number of U.S. seniors matched to family medicine positions rose by 11 percent over 2010. In Match Day ceremonies across the country today, these individuals will be among more than 16,000 U.S. medical school seniors who will learn where they are going to spend the next three to seven years of residency training.



Posted by
Aggravated DocSurg
at
2:26 PM
|
![]()
Friday, April 15, 2011
The Aggravated DocSurg Field Guide to the American Surgeon
I’m in Las Vegas. Actually, I was in Las Vegas, but because my swanky hotel didn't provide the basic internet service that your average Travelodge does, I didn't get to post this until now. Not my favorite place, to be honest --- I don’t gamble, smoke, or hang out with hookers.  The ads for “Kourtney Kardashian’s birthday party” at Planet Hollywood don’t interest me in the least. I’m quite sure that that mobile billboard advertising for “girls that want to meet” me are a bit less than honest. And I think it is frankly immoral to charge a guy $22 for a martini that isn’t served in a quart-sized glass.
The ads for “Kourtney Kardashian’s birthday party” at Planet Hollywood don’t interest me in the least. I’m quite sure that that mobile billboard advertising for “girls that want to meet” me are a bit less than honest. And I think it is frankly immoral to charge a guy $22 for a martini that isn’t served in a quart-sized glass.
This trip was about business, not pleasure. I was at the Trauma, Critical Care, and Acute Care Surgery meeting held at Caesar’s Palace every spring. Basically, it’s a meeting that talks about all of the things that you don’t want to have happen to you. I have a general rule about medical meetings --- never stay at the hotel hosting the event. The room rates are high, despite the advertisements for “discounted” prices in the meeting brochure, and I like to stretch my legs a bit on the way to and from the lectures. This provides me plenty of time to practice my people watching skills.
 This year, the trauma surgeon meeting was held one floor above a meeting for academic internists. Oil and water, so to speak. Being the slacker that I am, I didn’t bring along the meeting brochure with me to tell me where to go. And since Caesar’s wants people to wander and get mired in the casino, there were no signs directing me to the meeting this morning. So with a couple of thousand doctors streaming up the escalators to meeting rooms, how was I to tell where to go?
This year, the trauma surgeon meeting was held one floor above a meeting for academic internists. Oil and water, so to speak. Being the slacker that I am, I didn’t bring along the meeting brochure with me to tell me where to go. And since Caesar’s wants people to wander and get mired in the casino, there were no signs directing me to the meeting this morning. So with a couple of thousand doctors streaming up the escalators to meeting rooms, how was I to tell where to go? It’s simple. I know my peeps! I had no more trouble distinguishing the surgeons from the internists than a mother does her twins. And now, thanks to the Aggravated DocSurg Field Guide to the American Surgeon™, you too can know how to spot a surgeon in any environment.
The first clue to differentiating surgeons from internists at a meeting is a careful observation of how they walk --- surgeons are an impatient lot, and don’t tend to stand on escalators, wander, or stroll slowly. We tend to be on time, but just barely, and mostly arrive solo.
 Clothing is generally a bit rumpled, and at meetings older surgeons tend to adopt the same “uniform” --- khakis, a blue sport coat, and no tie. A quick glance at the wrist generally confirms a cheap watch --- Timex or Casio “nerd watch,” as SWIMBO calls them --- because we are always taking them off to scrub. Lost of loafers --- once again, because they have to be taken off frequently.
Clothing is generally a bit rumpled, and at meetings older surgeons tend to adopt the same “uniform” --- khakis, a blue sport coat, and no tie. A quick glance at the wrist generally confirms a cheap watch --- Timex or Casio “nerd watch,” as SWIMBO calls them --- because we are always taking them off to scrub. Lost of loafers --- once again, because they have to be taken off frequently. What about in the hospital? I know who everyone is at my place, but if somehow I was dropped into an ICU in Kalamazoo at midnight, and every doc in the place was wearing scrubs, it’s not really that hard. The surgeon in scrubs will unfailingly have messy hair from wearing a scrub cap all day, will be wearing some sort of OR-friendly shoes (Crocs, Danskos, etc.), more often than not is wearing a white coat, will roll his eyes a lot, and will have a feral look about him/her --- this is a deep-seated response to spending years in training where the hours were long and access to the next meal was suspect. If there’s a surgeon nearby, no doubt there’s a bit of food and coffee in the vicinity.
What about in the hospital? I know who everyone is at my place, but if somehow I was dropped into an ICU in Kalamazoo at midnight, and every doc in the place was wearing scrubs, it’s not really that hard. The surgeon in scrubs will unfailingly have messy hair from wearing a scrub cap all day, will be wearing some sort of OR-friendly shoes (Crocs, Danskos, etc.), more often than not is wearing a white coat, will roll his eyes a lot, and will have a feral look about him/her --- this is a deep-seated response to spending years in training where the hours were long and access to the next meal was suspect. If there’s a surgeon nearby, no doubt there’s a bit of food and coffee in the vicinity. The internist in scrubs looks a bit different --- wearing the same shoes he came to the hospital in, almost never in a white coat, carrying an armful of stuff that generally consists of patient lists, scribbled notes, and a laptop. But the single most distinguishing characteristic that marks the internist who is wearing scrubs is the presence of a stethoscope slung around his neck. This is as pathognomonic as the blue light special at K-mart.
The internist in scrubs looks a bit different --- wearing the same shoes he came to the hospital in, almost never in a white coat, carrying an armful of stuff that generally consists of patient lists, scribbled notes, and a laptop. But the single most distinguishing characteristic that marks the internist who is wearing scrubs is the presence of a stethoscope slung around his neck. This is as pathognomonic as the blue light special at K-mart.I hope this serves as a good introduction for those intrepid explorers who brave the halls of a hospital or who come across flocks of docs at a meeting place. The next edition of Aggravated DocSurg Field Guide to the American Surgeon™ will explore the finer points of surgeon identification, such as distinguishing residents from attendings, neurosurgeons from cardiothoracic surgeons, and the finer points of separating joint replacement orthopedists from hand surgeons based upon golf club brands.
If you are wondering if this guide is worthwhile, I can say I have already had one successful student -- Jimmy Buffett:
Posted by
Aggravated DocSurg
at
8:59 AM
|
![]()
Friday, March 25, 2011
Waiting & watching for Jon
We were invincible. Packed into Jon’s pale yellow Olds Cutlass, the car I’d always wanted, careening down the road between our high school and its “sister” all-girls school, we’d sing along with whatever was playing on the oversized speakers garishly mounted in the back. More exactly, we’d usually be screaming along with the music, which was loud enough to rouse more than a few nearby drivers from their afternoon daydreams.
We were on our way to......take a typing class. Twice a week, seniors who had asked for the class would get to spend a glorious hour pecking away at the Smith Corona keys. It was a treat, a privilege, something bestowed only on those who had grades that were up to par, and I’m sure some other selection process was at work as well. Even though there were no girls actually in the class at the time, we were surrounded by them.
And Jon was in his element.
Jon had one other arrow in his quiver, a gift from God, really. His eyes were the color of a Colorado winter sky, and brighter than a neon night. I suppose I’ve only seen something similar in movies, watching Grace Kelly or Paul Newman. But to see them in real life, in “action” so to speak, was remarkable. Personality plus pulsating blue eyes left the girls at Ursuline red-faced and giggling, and left the rest of us laughing, shaking our heads at how easily he could charm the pants off a nun.
Some time, somewhere later, Jon fell off a cliff. Looking back, as it always is, it is easy to recognize the direction he was headed. But the speed with which his drug problem took him down, and the depths to which it drug him, remains breathtaking to me even today. College was never completed --- hell, probably in reality never attempted. Having not seen him in several years, he showed up at my wedding, and then disappeared again, only to arrive unceremoniously at my doorstep with a pregnant girlfriend in tow. It was 11 PM, and I was dog-tired from working as a resident. And there he was, bright eyed as usual, but dirty, disheveled, and totally unaware of how badly he smelled.
That was 1990. I haven’t laid eyes on Jon since.
I know about the successive stents in drug rehab. I have had the opportunity to spend time with his ex-wife and children, and to learn of the tremendous loving influence his parents have had on them. And I have seen the pain in all of their faces, the ache in their voices. They, like me, miss Jon. But they have had to live with the person he became, and certainly don’t miss that guy.
I have put at least twenty versions of this down in electronic ink (those typing classes came in handy), and deleted them all. I have tried to write it in my head about a hundred times more. I guess I can’t come up with a way to end it, because there is no ending that will make me feel any better. Perhaps that is why I catch myself watching for Jon in places that I hope I might find him --- ski resorts, airports, restaurants when I go back to Dallas --- and more often in a place I fear I will find him --- in my ED.
We weren’t invincible.
Posted by
Aggravated DocSurg
at
1:20 PM
|
![]()
Saturday, February 19, 2011
It doesn't get any better than this -- America's mountain, a sunny day, and a mountain bike.
Posted by
Aggravated DocSurg
at
3:28 PM
|
![]()
Monday, February 14, 2011
Henny Penny in the Hospital
As much as I am not a fan of many of the studies that clutter medical journals --- poorly designed studies or those that display extreme bias --- I am occasionally delighted to find an article that is a bit out of the ordinary. It helps when it confirms my own biases (I admit it, I like to say "toldya so"), and there's an extra bonus for teaching me a new word. Such is the case for an article from the January edition of the American Journal of Surgery --- Catastrophizing: a predictive factor for postoperative pain.
 What the heck is catastrophizing? Well, it's listed in Dorland's medical dictionary (not in my prehistoric version, but in their online version), but I haven't been able to find it elsewhere. Put simply, catastrophizing is an irrational belief that something is far worse than it actually is. In the realm of pain research, pain catastrophizing is defined in the article as:
What the heck is catastrophizing? Well, it's listed in Dorland's medical dictionary (not in my prehistoric version, but in their online version), but I haven't been able to find it elsewhere. Put simply, catastrophizing is an irrational belief that something is far worse than it actually is. In the realm of pain research, pain catastrophizing is defined in the article as:...an exaggerated negative mental set brought to bear during an actual or anticipated painful experience (defined in simple words as expectation or worry about major negative consequences, even one of minor importance).
 OK, that means that some people worry excessively about pain associated with medical care, either during or before the actual care event. So? I worry about lots of things --- whether my kids will be alright when they are adults, whether or not I'll be able to bike to the top of the next hill without hacking up a lung, or whether SWIMBO will wake up one day and realize that she was duped into marrying me 23 years ago. I lay awake at night worrying about patients in the hospital, knowing that there is little I can do but wait. Well, in this situation, it's the degree of worry involved --- hence the provocative name for the problem. Once again from the article,
OK, that means that some people worry excessively about pain associated with medical care, either during or before the actual care event. So? I worry about lots of things --- whether my kids will be alright when they are adults, whether or not I'll be able to bike to the top of the next hill without hacking up a lung, or whether SWIMBO will wake up one day and realize that she was duped into marrying me 23 years ago. I lay awake at night worrying about patients in the hospital, knowing that there is little I can do but wait. Well, in this situation, it's the degree of worry involved --- hence the provocative name for the problem. Once again from the article,High levels of catastrophizing have been reported to be associated with a heightened pain experience and can result in the development of chronic pain.
- Pain catastrophizing is becoming recognized as a key predictor of the severity of acute post-surgical pain and its progression to chronic post-surgical pain. That's a big deal, because the severity of a patient's pain perception significantly alters their recovery and postoperative mobility, which can lead to other problems (DVT, atalectasis, etc.).
- There are screening tools available (the Coping Strategies Questionnaire and the Pain Catastrophizing Scale) to identify patients with a tendency to catasrophize, which could potentially allow us to tailor postoperative pain management for them.
Posted by
Aggravated DocSurg
at
10:04 AM
|
![]()
Wednesday, January 12, 2011
Tuesday, January 11, 2011
The OR Rorschach Test #8
For today's quiz, you need to be old enough to have read classic children's books, and young enough (at heart) to recognize a character:

--- if you are as old as I am, you gotta think Curious George when you see a monkey shape! Besides, Cheeta never played the piano, and though the Barenaked Ladies sing about chimpanzees, there's not actually one playing an instrument in their video.
Posted by
Aggravated DocSurg
at
9:23 AM
|
![]()
Tuesday, January 04, 2011
Snow White, RN and the Seven Surgeons
 Once upon a time, there was a princess who lived on the hospital surgical ward named Snow White, RN. She was beautiful, cheerful, helpful, efficient, and a damn good nurse. She took great care of her patients, and expected the same level of care from her compatriots. Naturally, that meant that she ran afoul the wicked witch, AKA the Queen Nurse, RN, BSN, PhD, QRS, ABC, etc. Fearing her independence and strengths, the Queen refused to promote Snow White, RN, to management. Every day, she would peer into her Blackberry to ask "
Once upon a time, there was a princess who lived on the hospital surgical ward named Snow White, RN. She was beautiful, cheerful, helpful, efficient, and a damn good nurse. She took great care of her patients, and expected the same level of care from her compatriots. Naturally, that meant that she ran afoul the wicked witch, AKA the Queen Nurse, RN, BSN, PhD, QRS, ABC, etc. Fearing her independence and strengths, the Queen refused to promote Snow White, RN, to management. Every day, she would peer into her Blackberry to ask "who is the ablest one of all who has filled in the most EBN matrix forms, completed the most forms on the EMR system, answered every question on the staff survey correctly, and doesn't ask "Who is that" on my semi-annual trips to the ward." Never seeing Snow White's name on the Blackberry, she was pleased; she did not need Snow White's heart in a jeweled box, because she was boxed in. (image source)

Dick Doc is the, well, you know...

Grumpy old Bastard is the general surgeon in his late 50s who has never seen an OR run more inefficiently, has never seen a room turnover in less than an hour, and looks like the barnacle encrusted crab that he is.

Hippie is the laid back surgeon who listens to Tales From Topographic Oceans during surgery. Thought he'd look like The Dude when he got to be 50, but looks a bit more like this dude instead.
Posted by
Aggravated DocSurg
at
10:20 PM
|
![]()
Monday, January 03, 2011
Billing Fraud or Documentation Errors?
I'm not really sure where it came from. Perhaps it started during medical school, where I funded dates with SWIMBO by typing lecture notes ($30 a pop for the shared lecture note service). Maybe it came later, trying to understand a patient's prior hospitalization reading someone else's notes that were so cryptic Mr. Turing would have had difficulty sorting through them. Regardless, I am sort of compulsive about documentation of my interactions with patients --- histories are always dictated as soon as I see a patient, operative notes are dictated as soon as I have spoken with the patient's family, etc. Even if I check on a (sick) patient half a dozen times during the day, I always leave a brief note in the chart.

Because the Government invests so much trust in physicians on the front end, Congress provided powerful criminal, civil, and administrative enforcement tools for instances when unscrupulous providers abuse that trust. The Government has broad capabilities to audit claims and investigate providers when it has a reason to suspect fraud. Suspicion of fraud and abuse may be raised by irregular billing patterns or reports from others, including your staff, competitors, and patients. When you submit a claim for services performed for a Medicare or Medicaid beneficiary, you are filing a bill with the Federal Government and certifying that you have earned the payment requested and complied with the billing requirements. If you knew or should have known that the submitted claim was false, then the attempt to collect unearned money constitutes a violation. A common type of false claim is “upcoding,” which refers to using billing codes that reflect a more severe illness than actually existed or a more expensive treatment than was provided.

It has created a new interagency task force called HEAT (Health Care Fraud Prevention and Enforcement Action Team) under which health-care officials will collaborate with the FBI to go after Medicare fraud. In addition, it has expanded to several cities the Medicaid Fraud Strike Force that authorizes FBI and Drug Enforcement Agency agents to jointly analyze Medicare claims data in real time to detect and investigate irregularities by area doctors. More chillingly, however, the administration is defining Medicare fraud down to include “unnecessary” and “ineffective” care. And to root this out, it plans to make expanded use of private mercenaries—officially called Recovery Audit Contracts—who will be authorized to go to doctors’ offices and rummage through patients’ records, matching them with billing claims to uncover illicit charges. What’s more, Obamacare increases the fine for billing errors from $11,000 per item to $50,000 without the government even having to prove intent to defraud.
That doesn't give me warm and fuzzies about "single payer" health care delivery in this country.
Posted by
Aggravated DocSurg
at
11:24 AM
|
![]()
Thursday, December 30, 2010
What a difference 1/6th of a day makes
A spectacular day in Colorado today ---- more accurately, a spectacular morning. When the sun is shining, 30 degrees feels like 50, letting Fat Boy get out for a little ride. This photo was taken at 10:00 this morning:
This afternoon --- not so spectacular. The view from my window right now, 4 hours after my ride:
Posted by
Aggravated DocSurg
at
2:07 PM
|
![]()
Sunday, December 19, 2010
The OR Rorschach Test #7
For your viewing pleasure, or puzzlement, today's OR Rorschach Test ---

Posted by
Aggravated DocSurg
at
11:21 AM
|
![]()
Friday, December 17, 2010
The OR Rorschach Test #6
Today's pop quiz --- what can you make of this OR Rorschach?

Posted by
Aggravated DocSurg
at
9:43 AM
|
![]()
Thursday, December 16, 2010
The OR Rorschach Test #5
 As always, your image interpretation mileage may vary.
As always, your image interpretation mileage may vary.
Posted by
Aggravated DocSurg
at
9:19 AM
|
![]()
Thursday, September 09, 2010
Operating Better, With Electricity!
 Sharp knives. Sutures. Hot lights and warm blood. Great music. That's what most folks picture when thinking about operating rooms. It's easy to overlook that we make use of plain old electrical energy in the OR --- electrosurgery. Sounds like something from a '50s SciFi novel. Perhaps a gift from the Red Lectroids from the 8th dimension?
Sharp knives. Sutures. Hot lights and warm blood. Great music. That's what most folks picture when thinking about operating rooms. It's easy to overlook that we make use of plain old electrical energy in the OR --- electrosurgery. Sounds like something from a '50s SciFi novel. Perhaps a gift from the Red Lectroids from the 8th dimension? 
Actually, the modern era of electrosurgery started in 1926, courtesy of Dr. William Bovie, a physicist, and Dr. Harvey Cushing, the father of neurosurgery in the US. The term "Bovie" is still standard jargon for the electrosurgical generator used in surgery, though most surgeons are only casually aware of its origins (there is a fair amount of history here and here, for those interested; image from Medscape). Me? Back in the dark ages, when (general, non-GYN) laparoscopic surgery was undergoing rapid growth and research opportunities abounded, I spent a year doing research, teaching laparoscopic surgery courses, and writing papers & book chapters. There had been considerable debate about the relative merits of using laser energy versus electrosurgery in laparoscopic gallbladder removal, and I landed the plum job of writing one of the papers that helped relegate laser laparoscopic cholecystectomy to the dustbin. Of course, as these things go, I also had many more writing assignments, including a book chapter entitled "Endoscopic Technology" for a book about laparoscopic and endoscopic surgery.
Let's just say, for someone who struggled to remember everything his father taught him about wiring a house, I learned quite a bit about electricity to write that chapter. And I learned even more about the potential for patient safety problems when using electrosurgery. For simplicity, though, the best way to think about electrosurgery is to picture a complete electrical circuit (image source):
 Any interruption in the circuit results in cessation of the flow of electrical energy (electrons). In the operating room, the "battery" is the electrosurgical generator, and rather than lighting a lamp, the energy is focused in the tip of an instrument, resulting in heat and tissue destruction, also called diathermy, where it is focused.
Any interruption in the circuit results in cessation of the flow of electrical energy (electrons). In the operating room, the "battery" is the electrosurgical generator, and rather than lighting a lamp, the energy is focused in the tip of an instrument, resulting in heat and tissue destruction, also called diathermy, where it is focused.OK, wait a minute. The generator is connected to the instrument, which is supposed to deliver electrical energy. But that doesn't make a complete circuit --- where is the rest of the circuit connecting back to the generator?
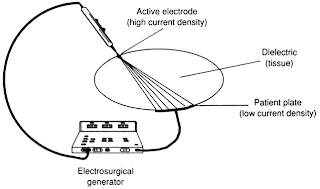 Well, a big chunk of the circuit is made, just like Soylent Green, of people! More accurately, of one person -- the patient --, to whom is attached a grounding pad (the passive electrode) that then connects back to the generator. Voila! A complete circuit is made, allowing high current density produced at the tip of the instrument (the active electrode) to cut and cauterize tissue.
Well, a big chunk of the circuit is made, just like Soylent Green, of people! More accurately, of one person -- the patient --, to whom is attached a grounding pad (the passive electrode) that then connects back to the generator. Voila! A complete circuit is made, allowing high current density produced at the tip of the instrument (the active electrode) to cut and cauterize tissue.
So what's different about using electrosurgery in laparoscopy? Well, a couple of things. First, we must use long instruments to reach the operative field, with an active electrode only at the tip of some of them. Second, those instruments must pass through trocars that maintain a seal to prevent the escape of CO2 from the inflated abdomen. And finally, we use a non-insulated telescope attached to a video camera to view what is happening in the operative field. As a result, there are many places where electricity may end up flowing other than where it is intended to be focused. If the active electrode/cautery tip is activated against an uninsulated portion of another instrument, tissue that is in contact with that instrument can be injured. If the cautery tip is activated out of view of the camera, it can result in unrecognized tissue injury. And there is a more complex problem called capacitive coupling, unique to laparoscopic surgery, that can result in tissue injury.
Perhaps the most pernicious risk, however, is insulation failure. Because we want action only at the tip of the active electrode, the remainder of the length of the instrument is insulated to prevent "leakage" of electricity ---- which can cause a tissue burn when the shaft of the instrument is laying against, for example, a piece of bowel, well out of view of the operative field. That risk, I have always felt, can be eliminated by using disposable rather than reusable cautery instruments. Additionally, the other instruments not actively delivering electrical injury may have insulation defects, and can similarly cause injury if they are used in contact with the active electrode/cautery.
Looks like I may be right for a change --- Insulation failure in laparoscopic instruments is a study published in Surgical Endoscopy earlier this year (unfortunately no unregistered access to article or abstract). Basically, the authors looked at reusable and disposable laparoscopic instruments used to deliver electrical energy and tested them for insulation defects. From the abstract:
Two hundred twenty-six laparoscopic instruments were tested (165 reusable). Insulation failure occurred more often in reusable (19%; 31/165) than in disposable instruments (3%; 2/61; p less than 0.01). When reusable sets were evaluated, 71% (12/17) were found to have at least one instrument with insulation failure. Insulation failure incidence in reusable instruments was similar between hospitals that routinely checked for insulation failure (19%; 25/130) and hospitals that do not routinely check for insulation failures (33%; 7/21; p = 0.16). Insulation failure was most common in the distal third of the instruments (54%; 25/46) compared to the middle or proximal third of the instruments (p less than 0.05).Hmmm. One in five reusable instruments was found to have an insulation failure. Cue The Doors:
One in five
No one here gets out alive, now
You get yours, baby
I'll get mine
Gonna make it, baby
If we try
Hold on. If this was a humongous problem, wouldn't general surgeons be seeing electrosurgical injuries from laparoscopic surgery on a weekly basis? Yep. And we don't. Perversely, I would say that is a bit of an issue ---- because this is seen very rarely, it is something about which one may be less than vigilant.
From my standpoint, I have a few things I insist upon when doing laparoscopic surgery; most importantly, I will only use disposable cautery instruments, as they are heavily used and most prone to insulation failure. Secondly, I don't use any other instruments to help deliver electrical energy/cautery; in open surgery, we frequently pick up a small bleeding vessel with a pair of forceps and then deliver the cautery against the forceps, delivering the electricity through them to the tissue that they hold --- for me, an absolute never in laparoscopic surgery. Finally, when appropriate I use alternate methods of delivering energy to tissues --- bipolar electrosurgery (that's another post) or high frequency ultrasonic energy most commonly.
In the end, the problem associated with insulation failure is really no different than many other potential pitfalls in medicine --- being well aware of the potential problem is the best method of its prevention.
Posted by
Aggravated DocSurg
at
4:02 PM
|
![]()























